The Economics of Oral Care: How Dentists Balance Quality, Cost, and Accessibility
Oral care shapes public health systems. It affects work, school, and daily comfort. The modern clinic faces tight budgets. Yet patients expect high standards. So, providers must balance value and care. The field blends science with business realities. The dentist works within these limits. Costs rise with new tools and training. However, access remains a social need. Elite Dental Center reflects this balance in practice.
Understanding the Cost Structure of Dental Care
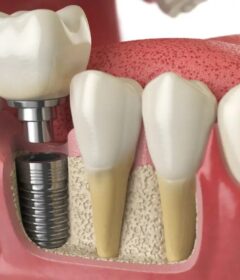
Dental clinics manage many fixed costs. Equipment requires large capital investment. Advanced imaging devices cost significant sums. Sterilization systems need constant maintenance. Rent and utilities add pressure. Staff salaries form a steady expense base. The clinic must also fund insurance and compliance requirements. Now each treatment carries overhead allocation. Materials like composites and implants are costly. Quality materials improve patient outcomes. However, they raise service prices. Elite Dental Center invests in modern systems. The aim is safety and efficiency. Financial planning guides all purchases.
Strategic Priority: Quality
Quality determines longevity. Patients want safe, long-lasting medicines. Clinic requirements must be met. Skilled workers need continuing training. Time and money are needed for training. That makes professional development an investment. Results are compatible with evidence-based practices. Quality assurance systems closely monitor results. Elite Dental Center stresses prevention. This method boosts patient loyalty.
Price And Affordability Pressures
Pricing needs rigorous consideration. Clinics measure local income. Market competition sets service prices. Fairness is the goal. However, affordability issues persist. Insurance coverage varies by region. Some plans restrict reimbursement. Clinics change service offerings. Pricing transparency boosts patient confidence. Payment plans help finances. The practice must not undercharge. Sustainable revenue aids clinical excellence. Controlling costs protects operational margins. Effective scheduling cuts chair time.
Accessibility and Community Responsibility
Access to care drives social equity. Rural areas often lack providers. Urban centers face long waiting times. The distribution of services remains uneven. Public health programs attempt to bridge gaps. Government subsidies influence treatment availability. So private clinics assess community needs. Outreach initiatives promote early screening. Sometimes mobile units serve remote neighborhoods. Partnerships with schools encourage preventive habits. The clinic balances charity with viability. Sliding scale fees support vulnerable groups. Service delivery is guaranteed by economic sustainability.
Innovation And Longevity
Technology changes dental treatment. Digital records simplify work. Automatic reminders cut missed visits. Data analytics aid resource allocation. Strategic planning is necessary. Prevention models generate steady revenue. From reactive to proactive care improves results and cuts costs. Supplier collaboration improves pricing. Continuous evaluation aids adaptation. Long-term value depends on patient retention.
Conclusion
The economics of oral care remain complex. Clinics operate within financial constraints. Quality cannot be compromised. Accessibility must remain a priority. So, balance defines professional success. Strategic investment supports clinical integrity. Thoughtful pricing encourages broader access. The careful blend of science and business shapes modern practice.